Few applications of emergency point-of-care ultrasound are more time critical and potentially lifesaving as cardiac ultrasound to detect pericardial tamponade.
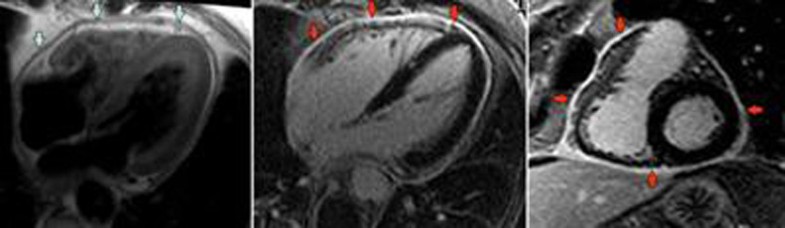
Physical exam findings, such as Beck’s triad (hypotension, jugular venous distention, and muffled heart sounds), although commonly emphasized, are not specific, and may be more reliable in trauma patients with a rapid accumulation of fluid. Bedside ultrasound allows rapid, noninvasive diagnosis of pericardial effusion and acute pericardial tamponade. Although the incidence of pericardial effusions in the general population is not known, data suggest that up to 13.6% of patients with otherwise unexplained dyspnea presenting to emergency departments have pericardial effusions of varied clinical significance. She was discharged on an oral course of levothyroxine with close follow-up with a cardiologist.Pericardial effusions are defined as the presence of fluid in the pericardial space that exceeds the upper physiologic amount of 50 mL and may be caused by malignancy, uremia, trauma, infection, and rheumatologic diseases. Repeat echocardiogram prior to discharge revealed significant improvement, showing only moderate effusion adjacent to the left ventricle. Following clinical improvement was transitioned to oral levothyroxine 100 mcg daily, and hydrocortisone was slowly discontinued. Also received hydrocortisone 50 mg every 8 hours. She was initially treated with a single dose of intravenous levothyroxine 300 mcg, followed by 100 mcg daily. A transthoracic echocardiogram confirmed a large circumferential pericardial effusion without tamponade physiology and severe concentric left ventricular hypertrophy (Figure 4).
#Trivial pericardial effusion free#
Thyroid-stimulating hormone (TSH) was 102.94 UIU/ML (normal range 0.30-5.50 UIU/ML) with a free T 4 less than 0.1 NG/DL (normal range 0.9-1.8 NG/DL). Imaging revealed cardiomegaly and pulmonary congestion on chest radiography (Figure 2), while computerized tomography (CT) chest with contrast revealed a moderate to large pericardial effusion (Figure 3). Initial workup revealed pancytopenia with macrocytosis and revealed an unremarkable chemistry panel with a brain natriuretic peptide (BNP) of 133.4 PG/ML.
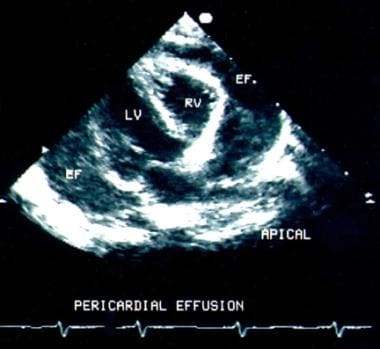
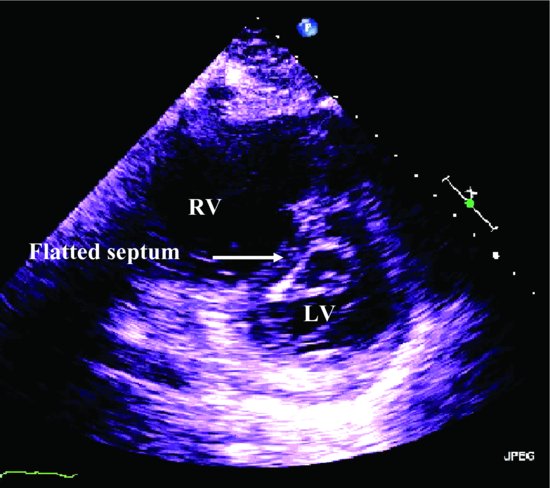
The examination revealed muffled heart sounds, jugular venous distention, and features consistent generalized myxedema (Figure 1).

She was awake, was appeared frail, and was not in acute distress. Initial vitals were notable for bradycardia and hypoxia, with an oxygen saturation of 80% necessitating supplemental oxygen. Question: What are the cardiac implications of untreated hypothyroidism?Īnswer: We present a case of pericardial effusion from primary hypothyroidism.Ī 70-year-old woman with a history of chronic obstructive pulmonary disease (COPD), chronic arthritis with no documented hypothyroidism presented to the emergency department with dyspnea evolving over the last month, generalized weakness, and arthritic pain. Early recognition and treatment can help mitigate these advanced features. Its cardiovascular manifestations include reductions in heart rate and contractility with the development of hypertension, angina, heart failure, and pericardial effusion consistent with hypothyroid heart. Primary hypothyroidism has been associated with many undue adverse effects.
